|
The corneal thickness is not uniform along the surface, neither pathologic nor healthy corneas. In the following lines, the main distinctive features allowing the clinician to distinguish PMD from the rest of ectatic disorders are described in detail. However, it is not always an easy task due to the similarities between some ectatic corneal disorders, especially in atypical manifestations of each of them. The differentiation between all ectatic disorders is clinically very relevant for a suitable management of each condition. Therefore, the corneal protrusion in PMD is then placed below the Differential diagnosis Likewise, the cornea frequently presents an area of increased curvature below this band. Classically, there is a flattening of the vertical meridian above the band of thinning, with the generation of a marked “against-the-rule” astigmatism. The hallmark of the disease is an inferior band of thinning 1 to 2 mm from the inferior limbus, although as previously commented, this band may be located on other positions. PMD is usually diagnosed in the later Typical clinical manifestation of PMD 
However, there are some disagreements between both conditions, such as age of presentation. Several authors have proposed that PMD is a peripheral form of keratoconus due to the close similarities between both conditions. Section snippets Etiologic and heritance factorsĬurrently, the exact etiology of PMD is unclear and it is not known whether PMD, keratoconus and keratoglobus are distinct diseases or represent different clinical presentations of the same underlying disease. According to epidemiological studies about the incidence of PMD, this condition is considered as a rare condition, less common than other ectatic diseases, such as keratoconus, but more common than others, such as keratoglobus or posterior keratoconus. Furthermore, it may be considerably underestimated because PMD is often misdiagnosed as keratoconus due to its close resemblance in the clinical presentation. The incidence or prevalence of PMD is not clearly reported in bio-statistical studies. The term “pellucid” means clear and was used by the first time by Schlaeppi to denote the clarity of the cornea and the absence of any scarring, lipid deposition or vascularization, despite the presence of ectasia. However, there are several reports showing PMD cases with involvement of superior, and even temporal and nasal regions of the cornea. This condition most commonly involves the inferior cornea, with a thinning extending from the 4-o´clock to the 8-o´clock positions. Pellucid marginal degeneration (PMD) is a non-inflammatory and progressive ectatic corneal disease characterized by a narrow band of corneal thinning separated from the limbus by a relatively uninvolved area 1–2 mm in width. 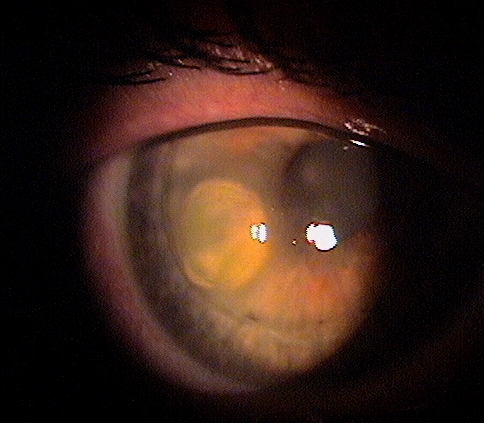
In addition, biomechanical and densitometric properties have been studied as complementary techniques to help in the diagnosis of PMD. New Scheimpflug imaging-based devices have shown the importance and usefulness of the pachymetric map for an appropriate diagnosis of PMD. Corneal topographic indices and the classical crab-claw topographic pattern cannot be used as the main tool to distinguish between PMD and keratoconus. 
Slit-lamp examination is very useful to distinguish PMD from other corneal ectatic disorders with inflammatory nature. PMD usually starts later in life than keratoconus and progresses slower than keratoconus. It is a rare corneal disorder that shares many clinical characteristics with other corneal ectasias, such as keratoconus, keratoglobus or Terrien marginal degeneration. Pellucid marginal degeneration (PMD) is a non-inflammatory ectatic corneal disease characterized by a narrow band of corneal thinning separated from the limbus by a relatively uninvolved area 1–2 mm in width.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
